Researchers developing a ‘universal’ flu vaccine
18 Dec 2013
Every year the approach of flu season sets off a medical guessing game with life or death consequences. There are many different strains of flu, and they vary from year to year. So each season authorities must make an educated guess and tell manufacturers which variants of the flu they should produce vaccines against.
 Even when this system works, flu-related illnesses can kill 3,000 to 49,000 Americans annually, according to the Centers for Disease Control and Prevention.
Even when this system works, flu-related illnesses can kill 3,000 to 49,000 Americans annually, according to the Centers for Disease Control and Prevention.
Recent estimates put the worldwide death toll from flu-related illnesses at between 250,000 and 500,000 people a year. A bad guess or the unexpected emergence of a virulent strain could send the death toll higher.
Against this backdrop Stanford researchers report promising steps toward the creation of a universal flu vaccine, one that could be produced more quickly and offer broader protection than the virus-specific inoculants available today.
The researchers detail their work in the current edition of the Proceedings of the National Academy of Sciences. The team was led by chemical and bioengineer James R. Swartz, who is the James H. Clark Professor in the School of Engineering.
Their approach arises from a better understanding of the structure of a key protein on the surface of the flu virus and a new process for making vaccines based on that understanding.
Professor James Swartz's team has made promising steps toward the creation of a universal flu vaccine. (Joel Simon)
A flu virus is made up of different proteins. Protruding from the surface of the virus are hundreds of copies of a protein called Hemagglutinin (HA). Each copy of HA resembles a mushroom, with a head and a stem. The head of HA helps determine the virulence of a given strain of flu.
Today's vaccines are based on inactivated viruses that contain the heads of HA proteins. When a flu shot is injected into the blood stream, the immune system sees the HA head as a target, and creates antibodies to fight what appears to be an infection.
 Teaching the immune system to recognize a target is the essence of vaccination. If we are exposed to the flu after being vaccinated, our immune system will be primed to recognize and eradicate the invading virus before it can replicate sufficient copies to make us sick.
Teaching the immune system to recognize a target is the essence of vaccination. If we are exposed to the flu after being vaccinated, our immune system will be primed to recognize and eradicate the invading virus before it can replicate sufficient copies to make us sick.
Swartz and his colleagues base their new vaccine approach on the understanding that, whereas the head of the flu virus varies from year to year, the protein stem remains more constant over time.
Theoretically, a vaccine based on the stem should be more broadly protective against different strains of flu and perhaps offer universal protection. Moreover, because the stem remains relatively constant from year to year, once the immune system produces antibodies against that antigen, multi-season protection might be possible.
This approach remains experimental and has not yet been tested on patients.
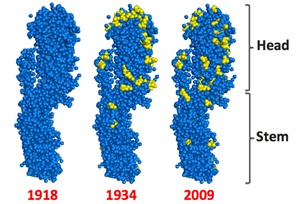
This image shows the HA protein from three flu strains. The HA protein is the target for current vaccines. It has a head and a stem. Current vaccines target the head. The blue and yellow dots depict the amino acids that make up the HA protein. The yellow dots show amino acids that change in the 1934 and 2009 protein relative to the 1918 variant. There are more changes in the head than in the stem.


















