Discovery paves way for home-brewed drugs, prompts call for regulation
20 May 2015
Fans of home-brewed beer and backyard distilleries already know how to employ yeast to convert sugar into alcohol. But a research team led by University of California at Berkeley (UC Berkeley) bio-engineers has gone much further by completing key steps needed to turn sugar-fed yeast into a microbial factory for producing morphine and potentially other drugs, including antibiotics and anti-cancer therapeutics.
 It may soon make growing fields of opium poppy unnecessary when it comes to the production of opiates and potentially other drugs, such as antibiotics. A team led by UC Berkeley bioengineers has completed key steps that will enable yeast to convert sugar into pharmaceuticals.
It may soon make growing fields of opium poppy unnecessary when it comes to the production of opiates and potentially other drugs, such as antibiotics. A team led by UC Berkeley bioengineers has completed key steps that will enable yeast to convert sugar into pharmaceuticals.
Over the past decade, a handful of synthetic-biology labs have been working on replicating in microbes a complex, 15-step chemical pathway in the poppy plant to enable production of therapeutic drugs. Research teams have independently recreated different sections of the poppy's drug pathway using E. coli or yeast, but what had been missing until now were the final steps that would allow a single organism to perform the task from start to finish.
In a new study that appeared on Monday, May 18, in the advanced online publication of the journal Nature Chemical Biology, UC Berkeley bioengineer John Dueber teamed up with microbiologist Vincent Martin at Concordia University in Montreal, to overcome that hurdle by replicating the early steps in the pathway in an engineered strain of yeast. They were able to synthesise reticuline, a compound in poppy, from tyrosine, a derivative of glucose.
''What you really want to do from a fermentation perspective is to be able to feed the yeast glucose, which is a cheap sugar source, and have the yeast do all the chemical steps required downstream to make your target therapeutic drug,'' says Dueber, the study's principal investigator and an assistant professor of bioengineering. ''With our study, all the steps have been described, and it's now a matter of linking them together and scaling up the process. It's not a trivial challenge, but it's doable.''
Paving the path from plants to microbes
The qualities that make the poppy plant pathway so challenging are the same ones that make it such an attractive target for research. It is complex, but it is the foundation upon which researchers can build new therapeutics. Benzylisoquinoline alkaloids, or BIAs, are the class of highly bioactive compounds found in the poppy, and that family includes some 2,500 molecules isolated from plants.
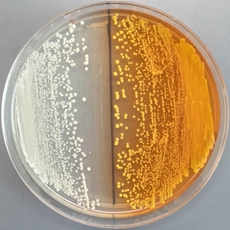 | |
| On the right are yeast cells producing the yellow beet pigment betaxanthin, which UC Berkeley researchers used to quickly identify key enzymes in the production of benzylisoquinoline alkaloids (BIAs), the metabolites in the poppy plant that could lead to morphine, antibiotics and other pharmaceuticals. (Photo by William DeLoache) |
''Plants have slow growth cycles, so it's hard to fully explore all the possible chemicals that can be made from the BIA pathway by genetically engineering the poppy,'' says study lead author William DeLoache, a UC Berkeley Ph.D. student in bioengineering. ''Moving the BIA pathway to microbes dramatically reduces the cost of drug discovery. We can easily manipulate and tune the DNA of the yeast and quickly test the results.''
The researchers found that by repurposing an enzyme from beets that is naturally used in the production of their vibrant pigments, they could coax yeast to convert tyrosine, an amino acid readily derived from glucose, into dopamine.
With help from the lab of Concordia University's Vincent Martin, the researchers were able to reconstitute the full seven-enzyme pathway from tyrosine to reticuline in yeast.
''Getting to reticuline is critical because from there, the molecular steps that produce codeine and morphine from reticuline have already been described in yeast,'' said Martin, a professor of microbial genomics and engineering. ''Also, reticuline is a molecular hub in the BIA pathway. From there, we can explore many different paths to other potential drugs, not just opiates.''
Red flag for regulators
The study authors noted that the discovery dramatically speeds up the clock for when homebrewing drugs could become a reality, and they are calling for regulators and law enforcement officials to pay attention.
''We're likely looking at a timeline of a couple of years, not a decade or more, when sugar-fed yeast could reliably produce a controlled substance,'' says Dueber. ''The time is now to think about policies to address this area of research. The field is moving surprisingly fast, and we need to be out in front so that we can mitigate the potential for abuse.''
In a commentary to be published in Nature and timed with the publication of this study, policy analysts call for urgent regulation of this new technology. They highlight the many benefits of this work, but they also point out that ''individuals with access to the yeast strain and basic skills in fermentation would be able to grow the yeast using the equivalent of a homebrew kit.''
They recommend restricting engineered yeast strains to licensed facilities and to authorized researchers, noting that it would be difficult to detect and control the illicit transport of such strains.
While such controls may help, Dueber said, ''An additional concern is that once the knowledge of how to create an opiate-producing strain is out there, anyone trained in basic molecular biology could theoretically build it.''
Another target for regulation would be the companies that synthesize and sell DNA sequences. ''Restrictions are already in place for sequences tied to pathogenic organisms, like smallpox,'' said DeLoache. ''But maybe it's time we also look at sequences for producing controlled substances.''
Other co-authors on this study are Zachary Russ and Andrew Gonzales of UC Berkeley's Department of Bioengineering, and Lauren Narcross of Concordia University's Department of Biology.




















